Pathophysiology of G6PD deficiency:
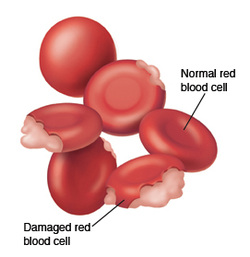
Hemolytic anemia is the most common medical problem that people with glucose-6-phosphate dehydrogenase deficiency are associated with. This happens when the red blood cells are destroyed at a much faster rate than which the body is able to replace them.
This is because G-6-PD is associated in supplying reducing energy to cells by maintaining the levels of the reduced form of the co-enzyme, nicotinamide adenine dinucleotide phosphate (NADPH), as it is the rate-limiting enzyme that converts glucose-6-phospate into 6-phosphoglucono-δ-lactone which supplies the reducing energy. Hence, NADPH maintains the supply of reduced glutathione in the cells which eliminates free radicals that are responsible for causing oxidative damage. As the only source of reduced glutathione in red blood cells is from the G-6-PD / NADPH pathway, the red blood cells which carries oxygen are at a risk of damage from oxidizing free radicals as the protective effect of glutathione is reduced. Therefore people with G-6-PD deficiency have a higher risk of hemolytic anemia in states of haemolytic stress.
Individuals suffering from this type of anemia may experience effects such as rapid heart rates, shortness of breath, yellowing of the skin and whites of the eyes or jaundice, paleness, dark urine and fatigue. The trigger for the hemolytic anemia in people with G-6-PD deficiency are often bacterial or viral infections as well as certain drugs like medications involved in treating malaria and some antibiotics. Additionally, consumption of fava beans, which are oxidants, or inhalation of fava plant pollen can also trigger the haemolytic anemia.
In severe cases, people with G-6-PD deficiency may experience acute renal failure. This is because in conditions of oxidative stress, all the remaining glutathione is consumed. As a result, proteins such as haemoglobin and enzymes are damaged by the oxidants which leads to electrolyte imbalance, cross bonding and protein deposition in the red cell membranes. Damaged red blood cells are then phagocytosed and sequestered in the spleen. Hemoglobin is then either metabolised to bilirubin which causes jaundice at high concentrations or excreted by the kidney in severe cases, causing acute renal failure.
Hemolytic anemia is the most common medical problem that people with glucose-6-phosphate dehydrogenase deficiency are associated with. This happens when the red blood cells are destroyed at a much faster rate than which the body is able to replace them.
This is because G-6-PD is associated in supplying reducing energy to cells by maintaining the levels of the reduced form of the co-enzyme, nicotinamide adenine dinucleotide phosphate (NADPH), as it is the rate-limiting enzyme that converts glucose-6-phospate into 6-phosphoglucono-δ-lactone which supplies the reducing energy. Hence, NADPH maintains the supply of reduced glutathione in the cells which eliminates free radicals that are responsible for causing oxidative damage. As the only source of reduced glutathione in red blood cells is from the G-6-PD / NADPH pathway, the red blood cells which carries oxygen are at a risk of damage from oxidizing free radicals as the protective effect of glutathione is reduced. Therefore people with G-6-PD deficiency have a higher risk of hemolytic anemia in states of haemolytic stress.
Individuals suffering from this type of anemia may experience effects such as rapid heart rates, shortness of breath, yellowing of the skin and whites of the eyes or jaundice, paleness, dark urine and fatigue. The trigger for the hemolytic anemia in people with G-6-PD deficiency are often bacterial or viral infections as well as certain drugs like medications involved in treating malaria and some antibiotics. Additionally, consumption of fava beans, which are oxidants, or inhalation of fava plant pollen can also trigger the haemolytic anemia.
In severe cases, people with G-6-PD deficiency may experience acute renal failure. This is because in conditions of oxidative stress, all the remaining glutathione is consumed. As a result, proteins such as haemoglobin and enzymes are damaged by the oxidants which leads to electrolyte imbalance, cross bonding and protein deposition in the red cell membranes. Damaged red blood cells are then phagocytosed and sequestered in the spleen. Hemoglobin is then either metabolised to bilirubin which causes jaundice at high concentrations or excreted by the kidney in severe cases, causing acute renal failure.
Content references:
http://ghr.nlm.nih.gov/condition/glucose-6-phosphate-dehydrogenase-deficiency
http://en.wikipedia.org/wiki/Glucose-6-phosphate_dehydrogenase_deficiency http://www.doctorslounge.com/hematology/diseases/g6pd.htm
Picture references:
http://www.vanderbilthealth.com/includes/healthtopics/article.php?ContentTypeId=3&ContentId=40319&Category=Hematology%20and%20Blood%20Disorders&SubtopicId=33128&lang=en§ion=33113 http://www.joy2taste.com/store/289/palace-deli-salted-broad-beans-in-ribbon-stripe/
http://www.rehcfl.com/blog/patient-education/do-you-have-symptoms-of-kidney-failure-symptoms-occur-when-your-kidney-function-is-less-than-15/
http://ghr.nlm.nih.gov/condition/glucose-6-phosphate-dehydrogenase-deficiency
http://en.wikipedia.org/wiki/Glucose-6-phosphate_dehydrogenase_deficiency http://www.doctorslounge.com/hematology/diseases/g6pd.htm
Picture references:
http://www.vanderbilthealth.com/includes/healthtopics/article.php?ContentTypeId=3&ContentId=40319&Category=Hematology%20and%20Blood%20Disorders&SubtopicId=33128&lang=en§ion=33113 http://www.joy2taste.com/store/289/palace-deli-salted-broad-beans-in-ribbon-stripe/
http://www.rehcfl.com/blog/patient-education/do-you-have-symptoms-of-kidney-failure-symptoms-occur-when-your-kidney-function-is-less-than-15/